Fewer tiny newborns are dying of intestinal necrosis, but many tragedies remain
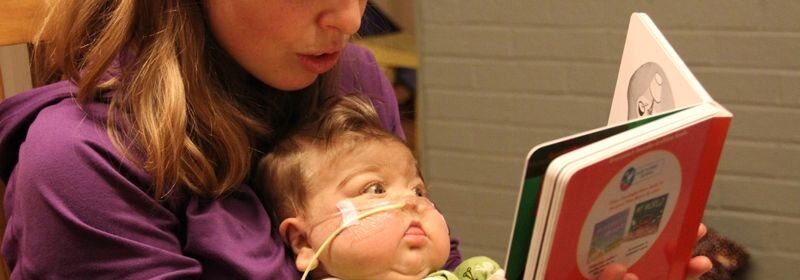
Jennifer Canvasser had never heard of necrotizing enterocolitis (NEC) before she gave birth to twins three months prematurely in 2011, but she has since devoted her life to raising awareness about this potentially fatal intestinal disease.
Her son Micah developed NEC when he was 6 weeks old and died of complications in December 2012.
He got sick quickly, and there were many ups and downs over the next 11 months, including multiple stints in the neonatal intensive care unit (NICU) and the pediatric intensive care unit.
“At 10 months, we thought he had made it, and then he developed pneumonia and got very sick,” Canvasser said. “Despite his bright smile and beautiful eyes, his body was just failing him because of complications.”
NEC primarily strikes premature and medically fragile infants like Micah. It happens when tissue in the small or large intestine is injured or inflamed. This can lead to death of intestinal tissue and sometimes a perforation in the intestine. Bacteria in the intestine can then travel into the bloodstream. Thousands of babies develop NEC in the United States every year, and hundreds die. Babies who do recover often face lifelong neurological and nutritional challenges.
To help spare others from the pain and loss that her family experienced, Canvasser founded the NEC Society in 2014.
“I was looking for a way to honor Micah by helping to build a world without NEC,” she explained.
While researchers have made strides in understanding, preventing and treating NEC, progress seems to have stalled, and racial and ethnic disparities still exist, according to new research published March 3 in JAMA Network Open.
For the study, researchers set out to see if U.S. death rates from NEC rose or fell between 1999 and 2020. Of more than 88 million live births during this period, 8,951 infants died of NEC.
NEC-related deaths declined by 7.7% each year from 2007 through 2012, but no further declines were seen, the study showed. While racial differences decreased over time, Black infants were still 2.5 times more likely to die from NEC than white infants in 2020.
“We still have a lot of work to do to reduce the rates of death from this disease,” said study co-author Dr. Ravi Patel, an associate professor of pediatrics at Emory University School of Medicine and Children’s Healthcare of Atlanta. “Too many babies are still dying from NEC.”
The exact cause of NEC still isn’t known, Patel said.
“We don’t know why babies develop it, but they have an immature intestinal system, and there may be a component of imbalance of bacteria in the gut,” he said.
The best ways to reduce NEC risk are breastfeeding or using human donor milk to feed infants.
“There are a lot of great things in human milk, including growth factors that protect the gut and probably influence the gut microbiome,” Patel said. (The gut microbiome reflects the balance of good and bad bacteria in the intestines.)
Canvasser, a study co-author, said it is also important for NICUs to partner with affected families to make sure they have everything they need to help babies with NEC.
Dr. Deborah Campbell, chief of neonatology at Children’s Hospital at Montefiore in New York City, said the findings mirror what she sees at her hospital, which serves predominantly Black and Hispanic patients.
“Through increasing focus on improving [before birth] outcomes for Black and other pregnant people of color and their infants, important strides have been made in improving maternal/birthing person and infant outcomes, though there remains significant work to be done,” she said.
The racial and ethnic gaps owe to a constellation of factors including interactions between biologic and social/environmental determinants of health—for example, access to medical care and being able to afford it.
Genetic variants that affect susceptibility to inflammatory events may also contribute to NEC risk and severity of the disease, Campbell said.
A diagnosis of NEC is challenging as there is no universal definition, and its exact cause is unknown, she said. Other conditions may mimic NEC in infants, including include bacterial or viral inflammation of the small intestine, intestinal obstructions or cow milk protein intolerance.
“There are no interventions that eliminate the risk for NEC in infants, although there are strategies that have been helpful in reducing the risk and severity of disease,” Campbell said. These include giving steroids to a pregnant patient who is at risk for preterm delivery; human milk feedings for the baby, and avoiding medications that may contribute to NEC, she said.
More information:
The NEC Society has more about NEC.
Journal information:
JAMA Network Open
Source: Read Full Article
