Calls ramp up for decriminalized hard drugs as B.C. breaks overdose death annual record
Nearly 1,500 British Columbians died of suspected illicit drug overdose deaths in 2018.
The BC Coroners Service reports 1,489 people died of drug overdoses compared to 1,420 illicit drug overdose deaths in 2017.
“Families and communities across the province are losing friends, neighbours and loved ones to illicit overdoses at an alarming rate,” B.C. chief coroner Lisa Lapointe said. “The illicit drug supply is unpredictable and unmanageable, and fentanyl is now implicated in 86 per cent of overdose deaths,” .
“The almost 1,500 deaths in B.C. in 2018 due to illicit drug overdoses far outweigh the numbers of people dying from motor vehicle incidents, homicides and suicides combined.”
WATCH (aired December 28, 2018): Vancouver to provide opioid pills to prevent overdoses
The coroner says drug overdoses have “plateaued” in British Columbia but the province is struggling to get a grip on the drug supply. Lapointe said fentanyl has been detected in 86 per cent of the illicit drug deaths.
The report shows that 77 per cent of the people who died were described as “regular or chronic users” of illicit drugs.
WATCH (aired January 31, 2018): Who is dying from illicit drug overdoses in B.C.?
“Not very often is it the person who goes to a party and uses for the first time and dies,” Lapointe said. “About four out of five of those who died had previous contact with the health-care system.”
Leading health authorities in the province have renewed calls for the decriminalization of hard drugs like opioids.
B.C. chief medial health officer Bonnie Henry says a drug clean supply would have significant impacts in savings lives.
The federal government is in charge of policy around drug legalization but the provincial government does have jurisdiction over prosecutions. Currently, B.C. is working on ways to prescribe prescription-grade heroin to drug users and provide other medications on a regular basis.
“What my office is looking at is how we can have de facto decriminalization for people who use drugs in B.C.,” Henry said.
“The federal government says they are very supportive on a number of issues but they are not at this moment looking at criminal code. But we cannot wait on the federal government to take those actions.”
Henry said the goal is to provide low-barrier access to a regulated supply of opioids and connect people who use drugs with the supports they need rather than sending them to the criminal justice system.
“If we’re going to turn the corner on this complex crisis, we need to find the ways to provide safer alternatives to the unregulated and highly-toxic drug supply and to end the stigma associated with criminalization of people who use drugs,” she said.
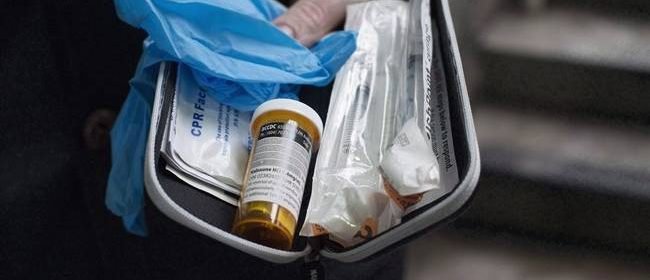
The B.C. government has been on the leading edge of addressing the ongoing drug epidemic. The province has made take-home naloxone kits available at over 1,480 locations, including almost 600 community pharmacies in the province.
There are now 21 overdose prevention sites in B.C., and nine supervised consumption sites are run by regional health authorities. According to the provincial government, over the past two years these sites were visited more than one million times with thousands of overdoses survived.
“My heart goes out to every family that has lost a loved one to overdose,” Mental Health and Addictions Minister Judy Darcy said. “This crisis truly shows us that people from all walks of life – professionals, people living in poverty, tradespeople and many other sectors – are all affected by addiction.”
“We are using every possible available tool to save lives, including a first-in-Canada pilot project at the St. Paul’s Hospital emergency department that provides people who have survived an overdose with take-home doses of suboxone and a well-defined treatment plan. This helps to stabilize people with opioid use disorder, ensuring they are connected to a safe alternative to toxic street drugs.”
The BC Centre on Substance Use is looking at including improved addiction training to support prevention and treatment.
Dr. Evan Wood, the organization’s executive director, says there is the need for policy changes to end prohibition, which creates the circumstances for the fentanyl market and continues to stigmatize substance use.
“This latest report confirms what those on the frontline already know all too well: this crisis is not slowing down,” Wood said.
“If we’re going to stop overdoses from happening, we urgently need to end the harms caused by prohibition while also implementing upstream responses that address the serious health and social consequences of untreated addiction.”
Source: Read Full Article

