Nursing Homes Are a Breeding Ground for a Fatal Fungus
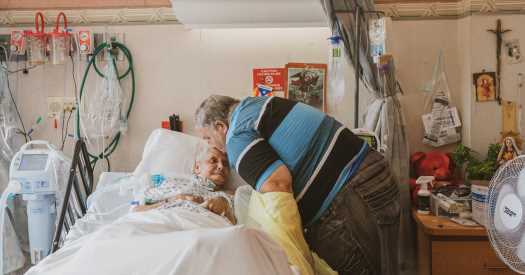
Maria Davila lay mute in a nursing home bed, an anguished expression fixed to her face, as her husband stroked her withered hand. Ms. Davila, 65, suffers from a long list of ailments — respiratory failure, kidney disease, high blood pressure, an irregular heartbeat — and is kept alive by a gently beeping ventilator and a feeding tube.
Doctors recently added another diagnosis to her medical chart: Candida auris, a highly contagious, drug-resistant fungus that has infected nearly 800 people since it arrived in the United States four years ago, with half of patients dying within 90 days.
At least 38 other patients at Ms. Davila’s nursing home, Palm Gardens Center for Nursing and Rehabilitation in Brooklyn, have been infected with or carry C. auris, a germ so virulent and hard to eradicate that some facilities will not accept patients with it. Now, as they struggle to contain the pathogen, public health officials from cities, states and the federal government say that skilled nursing facilities like Palm Gardens are fueling its spread.
“They are the dark underbelly of drug-resistant infection,” said Dr. Tom Chiller, who heads the fungal division at the Centers for Disease Control and Prevention, speaking about skilled nursing facilities, particularly those with ventilated patients, but not Palm Gardens specifically.
Such nursing homes are playing a key role in the spread in New York, where 396 people are known to be infected and another 496 are carrying the germ without showing symptoms, according to public health officials. In Chicago, half of patients living on dedicated ventilator floors in the city’s skilled nursing homes are infected with or harboring C. auris on their bodies, said Dr. Allison Arwady, the acting commissioner of the city’s Department of Public Health.
Much of the blame for the rise of drug-resistant infections like C. auris, as well as efforts to combat them, has focused on the overuse of antibiotics in humans and livestock, and on hospital-acquired infections. But public health experts say that nursing facilities, and long-term hospitals, are a dangerously weak link in the health care system, often understaffed and ill-equipped to enforce rigorous infection control, yet continuously cycling infected patients, or those who carry the germ, into hospitals and back again.
“They are caldrons that are constantly seeding and reseeding hospitals with increasingly dangerous bacteria,” said Betsy McCaughey, a former lieutenant governor of New York who leads the nonprofit Committee to Reduce Infection Deaths. “You’ll never protect hospital patients until the nursing homes are forced to clean up.”
[Read our other stories in our series on drug resistance, Deadly Germs, Lost Cures.]
The story is far bigger than one nursing home or one germ. Drug-resistant germs of all types thrive in such settings where severely ill and ventilated patients like Ms. Davila are prone to infection and often take multiple antibiotics, which can spur drug resistance. Resistant germs can then move from bed to bed, or from patient to family or staff, and then to hospitals and the public because of lax hygiene and poor staffing.
These issues have also vexed long-term, acute-care hospitals, where patients typically stay for a month or less before going to a skilled nursing home or a different facility.
A recent inquiry by the New York State Department of Health found that some long-term hospitals grappling with C. auris were failing to take basic measures, such as using disposable gowns and latex gloves, or to post warning signs outside the rooms of infected patients. At one unnamed facility, it said, “hand sanitizers were completely absent.”
Officials at the 240-bed Palm Gardens did not respond to repeated requests for comment. Over the past year, the number of patients who were infected with or were carrying C. auris there grew to 38 from six, according to a nurse there and public health officials. The tally has now fallen into the high 20s after some patients died or moved elsewhere.
The New York health department issued a statement in response to queries from The New York Times: “The Department of Health has made controlling the spread of C. auris a high priority and has conducted extensive training and education on infection control policies and procedures for Palm Gardens and other nursing home providers throughout this region. The health and well being of nursing home residents is our primary concern and we take complaints regarding quality of care very seriously.”
Scientific research on nursing homes and drug resistance is sparse, but some recent studies offer evidence of the problem. A study published in June in the Journal of Clinical Infectious Diseases found that patients and residents in long-term care settings have alarmingly high rates of drug-resistant colonization, which means they carry the germs on their skin or in their bodies, usually without knowing it, and can pass them invisibly to staff members, relatives or other patients. Elderly or severely ill people with weakened immune systems who carry the germ are at high risk of becoming infected. (Health officials in New York state said 14 percent of those now infected started out carrying it and then developed symptoms).
The study, which focused on Southern California, found that 65 percent of nursing home residents in that region harbored a drug-resistant germ, as did 80 percent of residents of long-term acute-care hospitals, where their “status is frequently unknown to the facility.” By comparison, only 10 to 15 percent of hospital patients carried such germs, the study found.
The phenomenon is global. A study published in 2017 found that elderly residents of long-term care facilities in Britain were four times as likely to be infected with drug-resistant urinary tract infections as elderly residents living at home. Soaring levels of resistance were found in long-term care facilities in Italy, a 2018 paper found. And a 2019 study found that long-term care facilities in Israel are “a major reservoir” of carbapenem-resistant Enterobacteriaceae, or CRE — a major family of drug-resistant germs — contributing to their “rapid regional dissemination.”
Experts said the problem is pronounced in the United States, given changing economics that push high-risk patients out of hospitals and into skilled nursing homes. The facilities are reimbursed at a higher rate to care for these patients, they said, providing an economic incentive for poorly staffed or equipped facilities to care for vulnerable patients.
C. auris, which is resistant to major antifungal medications, was first identified in 2009 in Japan and, as of July 31, had infected 796 people in the United States, largely in New York, Chicago and New Jersey, since its arrival here in 2015, according to the C.D.C. Another 1,540 people have been identified as carrying the germ on their skin or in their bodies without showing symptoms.
C. auris up close
On Palm Gardens’ second floor, where Ms. Davila and other ventilated patients reside, signs posted outside nearly every room warn visitors and staff members to wear gloves, gowns and masks — a state requirement for those infected with C. auris.
But during two recent visits to Palm Gardens by a Times reporter, accompanying Ms. Davila’s husband as his guest, orderlies and nurses moved in and out of her room without the required protection.
“The nurses and janitors are just spreading this thing from room to room,” her husband, Anthony Hernandez, said on a visit in August, shortly after a nurse, who was wearing gloves but no mask or gown, poured liquid nourishment into his wife’s feeding tube. During a brief interview in the lobby, Pamela Delacuadra, the center’s director of nursing, said employees had initially struggled with the infection-control protocols required for C. auris.
“It was overwhelming at first but with help from the health department, we’ve gotten much better,” she said.
Ms. Davila’s medical records, reviewed by The Times, do not identify the specific date when she got C. auris. But a chart written by a Palm Gardens doctor in December 2018 includes a note listing her as a carrier of the fungus. She was put in isolation for C. auris patients, and her records subsequently referred to her as having the infection and taking antifungal medications for it.
Palm Gardens occupies a nondescript seven-story brick building in a working-class neighborhood in central Brooklyn. Magenta banners promote its dialysis center and adult day care services, as well as a “respiratory pavilion” for patients on mechanical life support.
A high-level official from a local hospital that has seen a number of C. auris patients from nursing homes said Palm Gardens was a major source. He declined to be named because his employer had not authorized any comment.
Palm Gardens’s performance is poorly rated by the federal government; it received two stars, a below-average rating for staffing and overall care, from the Centers for Medicare and Medicaid Services, an agency that ranks nursing home care on a scale from one star to five. In 2018, the agency investigated the deaths of two ventilator patients at Palm Gardens, finding that employees had failed to turn their ventilators back on after performing mechanical checks. The patients died within minutes of each other, the report said.
C.M.S. declined to comment on Palm Gardens.
The ownership of Palm Gardens is controlled by someone identified as Shimon Lefkowitz, according to public filings.
Mr. Lefkowitz did not respond to efforts to reach him through Palm Gardens. Calls to several law firms that represent Palm Gardens in lawsuits were not returned.
Not all Palm Gardens residents with C. auris contracted the germ there, and it is not clear how many did. One patient who died was infected at Maimonides Medical Center in Brooklyn, according to the man’s family.
A changing role in health care
Skilled nursing homes and long-term care facilities have been playing an increasingly important role in caring for seriously ill patients who used to stay longer in hospitals.
Advances in medical technology have made it possible to prolong the lives of desperately ill patients, while changes in Medicare reimbursement rates created a financial incentive for the expansion of such facilities, said Neale Mahoney, an economist at the University of Chicago who studies the industry’s growth. There are now about 400 long-term care hospitals across the country, up from about 40 in the early 1980s, he said.
Since 2012, the number of skilled nursing homes with ventilator units rose to 436 from 367 — a significant jump but still a fraction of the nation’s 15,000 nursing homes — according to C.M.S.
“Ventilator units are the poster child, the best example of a place that has challenges,” said Dr. Alexander Kallen, an outbreak expert at the C.D.C.
The federal government reimburses facilities for ventilator patients at significantly higher rates than for other patients, according to C.M.S. Ventilated patients can bring in $531 a day compared to $200 for a standard patient. That’s about $16,000 a month compared to $6,000.
The reimbursement rates reflect the significant care required for vulnerable patients, and the cost of equipment.
C.M.S. contends the majority of skilled nursing homes do well with staffing and overall care. Yet roughly 1,400 nursing homes received a one-star rating for staffing in 2018 from the agency.
“It is impossible for them to do a good job with the way their staffing is,” said Dr. Mary Hayden, a professor at Rush Medical College who studies the rise of drug-resistant infections in health care, adding of the challenges of curbing drug-resistant infection: “The way they’re set up, they can’t do it.”
Ms. Davila’s path
Ms. Davila carried C. auris with her on her journey through the health care system.
In early August, after a routine blood test found her white cell count plummeting, she was taken by ambulance to Methodist Hospital in Brooklyn for a blood transfusion. Doctors discovered an infection and put her on two different antibiotics. Heavy use of antibiotics, while often necessary, can kill off the nonresistant infections and allow resistant ones to thrive.
Her condition stabilized after two weeks and she returned to Palm Gardens. It was one of at least a dozen trips she had taken to the hospital since she first arrived at Palm Gardens.
Her sharp decline began in 2017 after pain from a suspected hernia sent her to the hospital. A lifelong smoker, Ms. Davila had emphysema, which led to a litany of complications and infections, according to a review of her medical records.
Now she spends her days frozen in bed, serenaded by a Latin music radio station and the mechanical whir of her respirator.
Mr. Hernandez doubts his wife will recover. “If I can take her home to die that would be a blessing,” he said.
He pulled the blanket higher, turned up the radio and told his wife he loved her. Momentarily alert, she fixed her eyes on his and then mouthed: “I love you, too.”
Benjamin Ryan contributed reporting.
Andrew Jacobs is a reporter with the Health and Science Desk, based in New York. He previously reported from Beijing and Brazil and had stints as a Metro reporter, Styles writer and National correspondent, covering the American South. @AndrewJacobsNYT
Matt Richtel is a best-selling author and Pulitzer Prize-winning reporter based in San Francisco. He joined The Times staff in 2000, and his work has focused on science, technology, business and narrative-driven storytelling around these issues.
@mrichtel
Source: Read Full Article




