Maintenance dialysis patients may need additional shots of COVID-19 vaccines
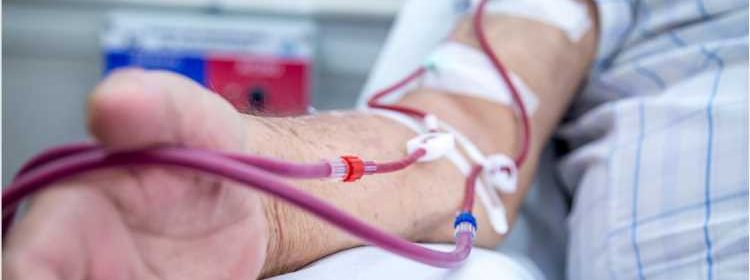
Researchers in the United States have conducted a study showing that the antibody response to vaccination designed to protect against coronavirus disease 2019 (COVID-19) wanes substantially over time among patients receiving maintenance dialysis.
The team’s study of more than 1,500 individuals found that antibody titers against the COVID-19 causative agent – severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) – rapidly dropped during the first six months following full vaccination.
Furthermore, the robustness of the initial response to vaccination appears to predict how quickly titers will wane.
Caroline Hsu from Tufts Medical Center in Boston, Massachusetts, and colleagues say that additional doses of COVID-19 vaccines should be considered for this vulnerable population.
A pre-print version of the research paper is available on the medRxiv* server, while the article undergoes peer review.
.jpg)
“Maintenance dialysis patients have an attenuated response to other vaccines”
The three COVID-19 vaccines currently authorized for use in the United States have all exhibited high efficacy in preventing death and serious illness in the general population.
However, concerns about the robustness and durability of the vaccine-induced immune response among vulnerable populations prompted the Centers for Disease Control and Prevention (CDC) to recommend a third dose for immunocompromised patients.
Currently, the implications for patients receiving maintenance dialysis are unclear and their inclusion within this classification depends upon the medical judgment of the treating clinician.
Early studies have shown that these patients initially generate an appropriate seroresponse to COVID-19 vaccination, although at a lower rate than among the general population.
“Given that maintenance dialysis patients have an attenuated response to other vaccines, with extensive data on additional or booster doses for hepatitis B vaccination, similar concerns exist that potential uremia-associated immunocompromise may impact the response to SARS-CoV-2 vaccines,” writes Hsu and colleagues.
What did the researchers do?
The team conducted a retrospective multicenter study to assess the seroresponse among 1,898 maintenance dialysis patients who were fully vaccinated against COVID-19.
Titers of immunoglobulin G (IgG) antibodies against the receptor-binding domain of the SARS-CoV-2 spike protein (SAb-IgG titers) were measured monthly and followed over time by prior history of COVID-19 and the type of vaccine received.
The spike protein mediates the initial stage of the infection process when its RBD binds to host cell receptors. This surface structure is a primary target of antibodies following natural SARS-CoV-2 infection or vaccination.
.jpg)
SAb-IgG titers declined over time following vaccination
Among 1,567 patients with no previous history of COVID-19, SAb-IgG titers declined over time following vaccination.
Of 441 individuals who received the BNT162b2 vaccine developed by Pfizer-BioNTech, the median SAb-IgG titer declined from 20 U/L during the first month to 2.69 U/L by month 4 and 1.30 U/L by month 6.
For 779 recipients of Moderna’s mRNA-1273 product, the corresponding titers were 20, 20 and 6.20, while 347 recipients of Janssen’s Ad26.COV2.S vaccine had a median titer of less than 1 U/L across all time periods.
In a time-to-event analysis, recipients of the Janssen product had the shortest time to loss of seroresponse (SAb-IgG less than 1 U/L) and Moderna vaccines recipients had the shortest.
The maximum titer reached in the first two months following full vaccination was predictive of the durability of the seroresponse. Patients who had a maximum initial SAb-IgG titer between 1 and 19.99 U/L were more likely to experience loss of seroresponse than those with a titer of 20 U/L or more.
“Additional doses of vaccine should be considered for this vulnerable population”
The researchers say the data provide longitudinal evidence that vaccine-induced immunity wanes rapidly among patients receiving maintenance dialysis.
“These data estimate that even following current vaccination standards, about half of maintenance dialysis patients will have suboptimal vaccine-induced protection in the fall of 2021, a time of projected high community prevalence of COVID-19,” they write.
The team says the current CDC recommendation to provide a third vaccine dose to immunocompromised patients is an important consideration for the maintenance dialysis population.
“Additional doses of vaccine should be considered for this vulnerable population, whether routinely or, with further investigation, potentially guided by protective correlates such as antibody response,” concludes Hsu and colleagues.
*Important Notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
- Hsu C, et al. Seroresponse to SARS-CoV-2 vaccines among maintenance dialysis patients over six months, medRxiv, 2021. doi: https://doi.org/10.1101/2021.09.13.21263535, https://www.medrxiv.org/content/10.1101/2021.09.13.21263535v1
Posted in: Child Health News | Men's Health News | Medical Research News | Medical Condition News | Women's Health News | Disease/Infection News
Tags: Antibodies, Antibody, Cell, Coronavirus, Coronavirus Disease COVID-19, Dialysis, Efficacy, Hepatitis, Hepatitis B, Immune Response, immunity, Immunization, Immunoglobulin, Protein, Receptor, Research, Respiratory, SARS, SARS-CoV-2, Severe Acute Respiratory, Severe Acute Respiratory Syndrome, Spike Protein, Syndrome, Vaccine

Written by
Sally Robertson
Sally first developed an interest in medical communications when she took on the role of Journal Development Editor for BioMed Central (BMC), after having graduated with a degree in biomedical science from Greenwich University.
Source: Read Full Article