Finding clues to nephronophthisis in adults
Nephronophthisis (NPH) is a kidney disease affecting mainly children. Now, for the first time, researchers at Tokyo Medical and Dental University (TMDU) have studied a number of adults with NPH and highlighted clinical, genetic and pathological characteristics that could help in confirming this challenging diagnosis.
NPH is inherited in an autosomal recessive pattern and, though rare, is the commonest genetic cause of kidney failure in children. The name is derived from ‘nephron’, the functional filtration units of the kidney and ‘phthisis,’ Greek for ‘wasting away.’ Recent genetic studies have highlighted that NPH may also present in adults resulting in end-stage renal disease (ESRD). However, there are only a few case-reports and no cohort studies, possibly because of rarity and diagnostic difficulties.
The clinical diagnosis of adult NPH is problematic because clinical, radiologic and histologic features are non-specific. Even the extrarenal features are fewer in adults. Because management includes renal transplantation and genetic counseling, an accurate early diagnosis is essential. Takuya Fujimaru, first author, explains further. “At present, molecular genetic analysis is the only practical method for clinically diagnosing NPH. However, as over 25 genes have been identified, Sanger sequencing (one DNA fragment at a time) is tedious; comprehensive mutation analysis using next generation sequencing (NGS) capable of sequencing millions of fragments is therefore required. Unfortunately, NGS is expensive and has limited availability. We therefore aimed to investigate the genetic background of adult nephronophthisis and evaluate the clinical characteristics and pathological changes in these patients.”
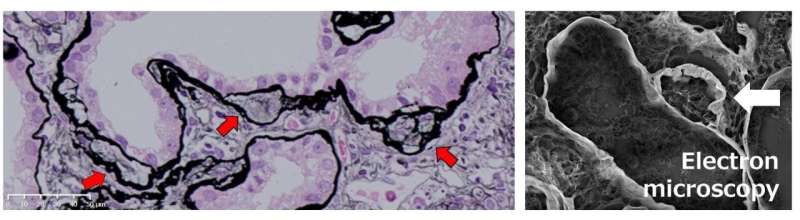
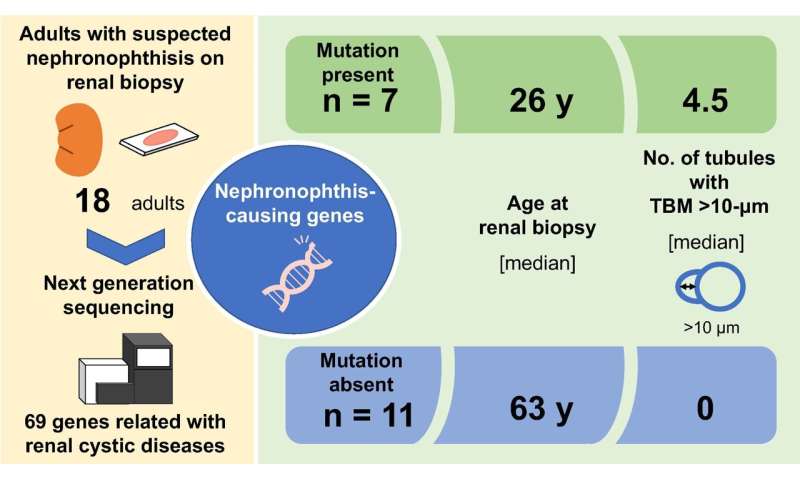
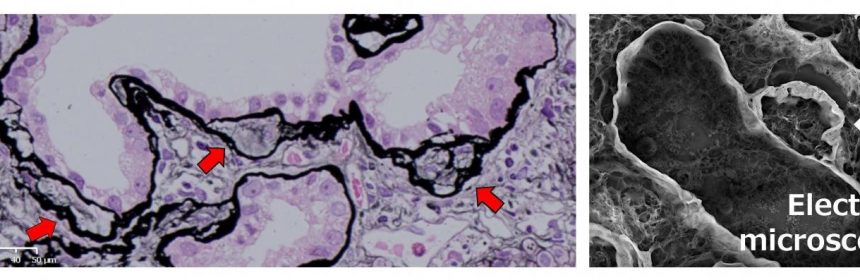
The research team, drawn from top medical institutions across Japan, studied 18 patients with adult-onset NPH suspected from kidney biopsy using cutting-edge tools such as low-vacuum scanning electron microscopy and capture-based sequencing. They analyzed 69 genes associated with kidney disease and compared patients with and without mutations. Seven of their patients had NPH-causing mutations; they were comparatively young though not significantly different in classic pathological findings. Interestingly however, thick tubular basement membrane (TBM) duplication was seen in many more tubules in these genetically proven patients.
Source: Read Full Article